At Nephrology Associates of Central Pennsylvania, Inc. our experienced doctors can treat all kidney related conditions including chronic kidney diseases, acute kidney disease or injury, dialysis, glomerular disease and nephrosis. Regular visits to your nephrologist can go a long way in preventing renal disease/ slowing down its advancement.
What is a Nephrologist?
A nephrologist is a physician that specializes in kidney health and kidney disease. Nephrology is a subspecialty of internal medicine. Therefore, a nephrologist would complete the same training as an internist and then complete an additional fellowship in nephrology.
Patients are commonly referred to a nephrologist for protein in the urine, elevated creatinine, electrolyte abnormalities, kidney stones, fluid overload, elevated blood pressure, acute kidney injury, and chronic kidney disease.
Chronic Kidney Disease (CKD)
Your kidneys are bean shaped organs and about the size of a fist. They are located in the middle of your back, on the left and right of the spine. The kidneys are attached to your bladder by tubes called ureters and the ureters carry urine to the bladder.
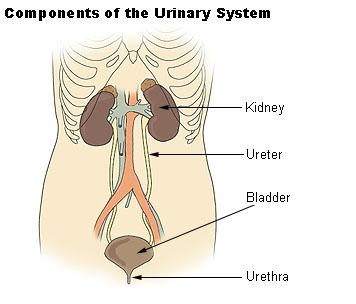
Functions of the kidney
- Filter your blood and remove extra water and waste to make urine
- Regulate your body water and chemicals in your blood such as sodium, potassium, phosphorus, and calcium
- Remove drugs and toxins introduced into your body
- Release hormones into your blood to help your body
- These hormones regulate blood pressure, make red blood cells, and promote strong bones
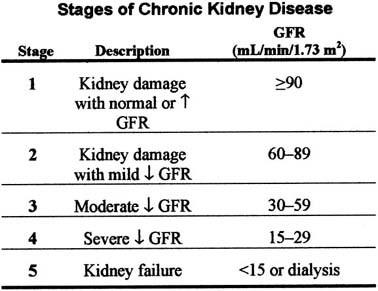
Chronic kidney disease means the kidneys have been damaged and are not able to keep you healthy. If kidney disease gets worse, wastes can build to high levels in your blood and make you feel sick. There are 5 stages of Chronic Kidney Disease (see image below).
Causes of kidney disease
Two main causes
- Diabetes or elevated blood sugars
- Happens when your blood sugar is too high, causing damage to many organs and muscles in your body, including the kidney, heart, blood vessels, nerves, and eye.
- Occurs when the pressure of your blood against the walls of your blood vessels increase.
- If not well controlled, it can cause heart attacks, strokes, and chronic kidney disease
Other causes.
- Glomerulonephritis
- Group of diseases that cause inflammation and damage to the kidney’s filtering units
- Inherited diseases such as polycystic kidney disease
- Immune diseases such as Lupus
- Malformations that occur as a baby develops
- Obstructions
- Caused by problems like kidney stones, tumors, or an enlarged prostate in men
- Repeated urinary infections
Symptoms of CKD
- Feel more tired and have less energy
- Trouble concentrating
- Decreased appetite
- Insomnia
- Fluid retention
- Dry, itchy skin
- Increased urination, especially at night
Testing for CKD
- Urine test for protein. Having protein in your urine can mean that your kidneys are not filtering your blood well. This can be a sign of kidney disease.
- Blood test for creatinine. When the kidneys are damaged, they have trouble removing creatinine from your blood.
- Blood test for Glomerular Filtration Rate (GFR). The creatinine is part of a math formula with your age, race, and sex to find out your GFR. The GFR helps determine the stage of kidney disease.
Treatment of CKD
The treatment of Chronic Kidney Disease depends on the stage of kidney disease and other health problems. The treatment plan would include treating the cause of kidney disease, managing any complications of kidney disease, and encouraging a healthy life style (exercise and diet program, controlling weight and high cholesterol, and smoking cessation).
Acute Kidney Injury (AKI)
Acute kidney injury is a sudden loss of kidney function that happens within a few hours or a few days. During AKI wastes and fluids can build up in the body. This can also affect other organs such as the brain, heart, and lungs. AKI is common in patients who are in the hospital, in intensive care units, and especially in older adults. Some causes of AKI include:
- Severe infections
- Some medications such as antibiotics
- Obstructions such as blockages in the urinary tract or enlarged prostate
- Severe burns
- Heart surgery
- Low blood pressure
- Decreased or blocked blood flow to the kidneys
The treatment plan for AKI would include treating the cause of AKI. If the kidney do not start to work on their own dialysis or other treatments may be needed.
Dialysis
- If your GFR falls below 15, you may need to start treatment for kidney failure
- Treatments include:
- Hemodialysis
- Peritoneal Dialysis
- Kidney Transplantation
- Declining or Withdrawing from treatment
Hemodialysis
Hemodialysis cleans and filters your blood using a machine to temporarily rid your body of harmful wastes and extra water. During your treatment, your blood travels through tubes into the dialyzer, which filters out wastes, extra salt, and extra water. Then the cleaned blood flows through another set of tubes back into your body. Hemodialysis can be done at an outpatient center or at home.
An access to your bloodstream will need to be created before your first hemodialysis treatment. This access provides an efficient way for blood to be carried from your body to the dialysis machine and back without causing discomfort.
The two main types:
- Fistula
- This is the preferred vascular access for Hemodialysis.
- A Vascular Surgeon makes a fistula by connecting an artery to a vein in your arm. The increased blood flow makes the vein grow larger and stronger so it can be used for hemodialysis. It may take several weeks to be ready for use.
- Graft
- A Vascular surgeon connects an artery to a vein by using a synthetic tube. It doesn’t need to develop as a fistula does, so it can be used sooner.
- Catheter
- A Catheter is typically used for temporary access due to the risk of infection with long term use. It is a small, soft tube that is inserted into a vein in your neck, chest, or leg near your groin.
In-center Hemodialysis
This treatment is done 3 days per week and can last approximately 3-5 hours. Some centers offer Nocturnal Hemodialysis. This treatment is done for approximately 6-8 hours at night, while you sleep at the center.
Home Hemodialysis
Hemodialysis can be done at home after a 6 week training course. This treatment can be done 3-7 days per week and is done by the patient with assistance from a family member, friend or caregiver.
Peritoneal Dialysis
Peritoneal dialysis cleans and filters your blood by using the peritoneal membrane (the lining of the abdomen). During the treatment a dialysis solution, which is a mixture of minerals and sugar dissolved in water, travels through a catheter into your abdomen. The sugar draws wastes and extra water from the tiny blood vessels in your peritoneal membrane into the dialysis solution. After several hours, the used solution is drained from your belly through a tube. Then your abdomen is refilled with fresh dialysis solution and the cycle is repeated.
There are 2 types of Peritoneal Dialysis: Continuous ambulatory peritoneal dialysis (CAPD) and Continuous cycler-assisted peritoneal dialysis (CCPD). Both types are considered a self-treatment that is done at home.
CAPD
CAPD does not require a machine and can be done in any clean, well-lit place. Most people change the dialysis solution at least 4 times a day and sleep with the solution in their abdomen at night. The treatment is done 7 days per week.
CCPD
CCPD uses a machine called a cycler to fill and empty the abdomen during the night while you sleep. The treatment is done 7 days per week.
High Blood Pressure
High blood pressure is also called hypertension. Blood pressure is the force of your blood against the walls of your blood vessels as your heart pumps blood around your body. If your pressure becomes too high, you are said to have high blood pressure.
High blood pressure is a leading cause of chronic kidney disease. Over time high blood pressure can damage blood vessels throughout the body and reduce the blood supply to the kidneys and other organs.
The treatment plan for high blood pressure includes a combination of life-style changes including a healthy diet, exercise, weight loss and smoking cessation. Many people with high blood pressure will also need medication to help lower their blood pressure.
Electrolyte Disorders
Potassium
Potassium is a mineral that helps your muscles and heart work properly. Too much or too little potassium in the blood can be dangerous.
Large amounts of potassium are found in:
- Certain fruits and vegetables
- Milk and yogurt
- Bananas, melons, oranges, potatoes, tomatoes, dried fruits, nuts, avocados, deep colored and leafy green vegetables, and some juices
- Milk and yogurt
- Dried beans and peas
- Most Salt substitutes
- Most protein-rich foods such as meat, poultry, pork and fish
Calcium
Calcium is a mineral that is important for building strong bones and teeth. It also helps muscles work properly. Disruptions in calcium can happen when the kidneys do not work properly.
- Calcium is found in:
- Milk, yogurt, and cheese are rich sources
- Vegetables such as broccoli, kale, baked beans
- Fruits such as apricots, figs, and oranges
- Calcium fortified foods such as fruit juices and drinks, tofu, and cereals
Calcium supplements should only be taken if recommended by your doctor.
Phosphorus
Phosphorus is a mineral found in food that helps your body use energy and helps build strong bones and teeth. Phosphorus can build up in your blood when your kidneys do not work properly. This can cause your calcium levels in your blood to drop. Calcium is then pulled from your bones to stabilize the calcium in your blood. Over time this can cause the bones to become weak and increase risk of bone fractures and bone pain.
- Large amounts of phosphorus are found in:
- Dairy products such as milk, cheese, yogurt, ice cream, and pudding
- Nuts and peanut butter
- Dried beans and peas
- Beverages such as cocoa, beer, and dark cola drinks
If your phosphorus becomes elevated in your blood you may need to limit phosphorus-rich foods and take a type of medicine called a phosphate binder.
Sodium
Sodium is a mineral found in most foods. Your body needs sodium for healthy nerves and to balance fluid levels. When the kidneys do not work properly, sodium and fluid can build up in the body. This can lead to elevated blood pressure and swelling in the body.
Sodium is found in large amounts in table salt and in foods that have added table salt such as:
- Seasonings like soy sauce, garlic salt, or onion salt
- Sauces like barbecue sauce, steak sauce, soy sauce, and oyster sauce
- Most canned foods and frozen dinners
- Processed meats like ham, bacon, sausage and cold cuts
- Salted snack food like chips and crackers
- Canned or dehydrated soups like packaged noodle soup
- Most restaurant foods, take-out foods, and fast foods
Tips for a low sodium diet
- To enhance the flavor of foods try fresh or dried herbs and spices
- Read food labels to help you choose foods with less sodium
Protein in the urine
Protein in the urine is also called proteinuria. Having protein in your urine can mean that your kidneys are not filtering your blood well. This can be a sign of kidney disease.
Kidney Stones
A kidney stone is a hard object that is made from chemicals in the urine. The stone-forming chemicals are calcium, oxalate, urate, cystine, xanthine, and phosphate. A kidney stone may stay in the kidney or travel down the urinary tract into the ureter. Sometimes, tiny stones are removed from the body in the urine without causing too much pain. Stones that do not move may cause a back-up of urine in the kidney, ureter, bladder, or urethra. This is what causes the pain.
Diagnosis of a kidney stone usually includes imaging tests to find out the exact size and shape of the kidney stone. Treatment may include increasing the intake of water and/or medication to help make the urine less acid. Surgery is indicated if a kidney stone is to large, if it blocks the flow or urine, or if there is a sign of infection.
Stone analysis may be completed to help determine why you have the kidney stone and how to reduce the risk of further stones.
Fluid retention
One function of the kidneys is to balance fluid in the body. If too much fluid builds up in your body, you can have fluid retention. This is commonly called fluid overload or hypervolemia. Fluid overload can cause elevated blood pressure, swelling, shortness of breath, and heart problems.
Fluid overload can be treated by medications called diuretics along with fluid and salt restrictions. In severe cases some people need dialysis to remove the fluid.
Kidney Disease Education
We provide patient-centered education classes for our patients with chronic kidney disease. Topics include chronic kidney disease, diabetes, high blood pressure, conditions related to kidney disease, nutrition, and depression. Modality classes are also offered to discuss treatment options including: hemodialysis, peritoneal dialysis, and kidney transplant.